THE NeuroPongTM PROGRAM – Parkinson’s Disease
Understanding Parkinson's Disease and Its Impact
Parkinson’s Disease (PD) is a chronic, progressive neurological condition impacting the planning, initiation, and control of movement. With over 10 million affected globally, it’s the second most common neurodegenerative condition. In the United States, about 1 million individuals live with Parkinson’s, with an estimated increase to 1.2 million by 2030. Though typically affecting those over 60, approximately 4% are diagnosed before 50. While genetics may play a role in 5-10% of cases, sporadic instances arise from a mix of environmental and genetic factors. Men face a 1.5–2 times higher risk than women.
What Leads to the Loss of Dopamine?
Causes of Parkinson’s Disease
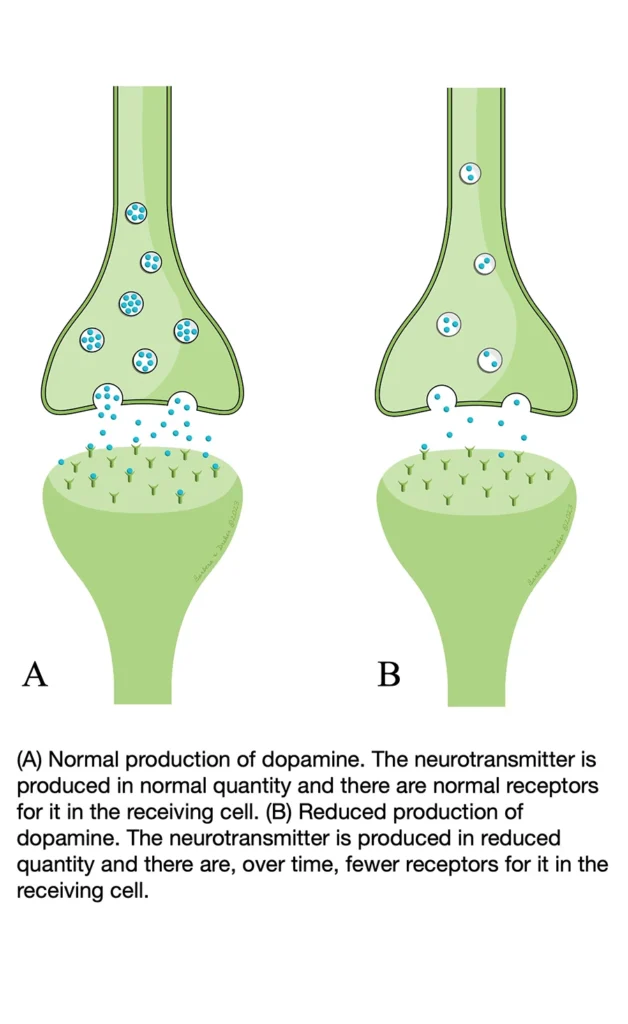
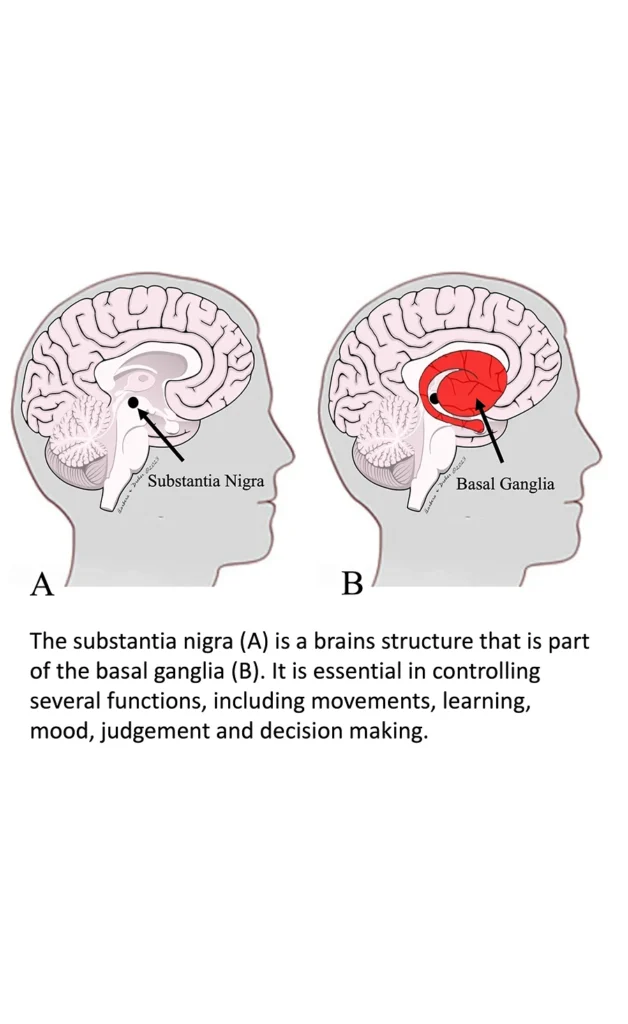
The death of the cells of the substantia nigra, as well as other areas of the brain and spinal nerves, leads to a reduction of dopamine and other neurotransmitters. The consequence of this affects both the somatic system (such as muscle movement) and autonomic system (blood pressure, nerve transmission, intestinal function, hormones, etc.), leading to motor and non-motor symptoms.
Even if the role of dopamine in enabling motor behavior is not well understood, the loss of the dopamine- containing cells leads to profound deficits in initiating, controlling, and maintaining movements.
Recognizing Motor & Non-Motor Symptoms
Clinical Presentation of Parkinson’s Disease
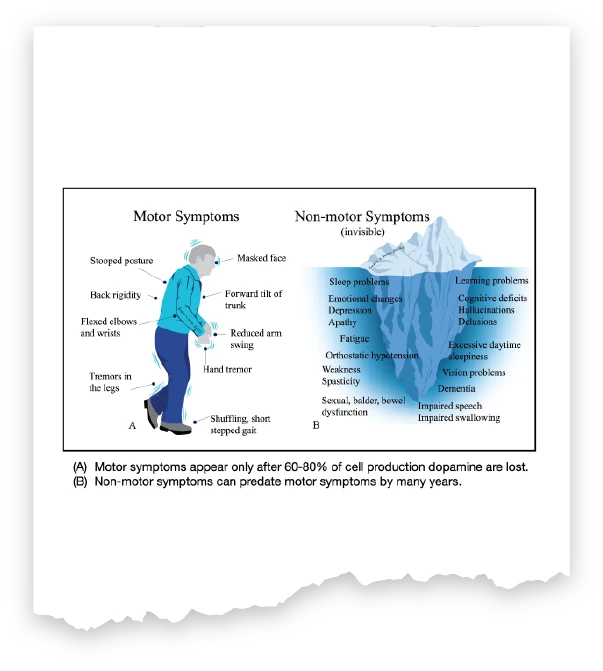
Primary symptoms include bradykinesia (slow movements), rigidity, tremors (usually found more at rest than with activity), dystonia (involuntary and painful muscle contractions), and postural instability, often resulting in balance issues and falls, which sometimes can be fatal. Non-motor symptoms, such as cognitive impairment and mood disorders, significantly impact quality of life.
Other motor symptoms include the loss of facial expression, known as mask face, micrographia (small handwriting), loss of manual dexterity, soft speech, taking smaller and faster steps or shuffling, or difficulty swallowing. “Freezing” describe problems with initiating movements in the legs and is often described as feeling like a person’s feet are stuck to the floor. It can occur when an affected person tries to walk, turns, or navigates through tight and crowded spaces.

Addressing Postural Instability Through Exercise
Balance Control and NeuroPong™
Balance control is an important priority in the NeuroPongTM program, with many of the program’s exercises aiming at increasing strength, balance and control during movements at the table tennis table. Two things about people with Parkinson’s to be aware of are ‘retropulsion’, which is a tendency to fall backward, and ‘propulsion’, which is the tendency to fall forward.
Varying Symptoms and Medication Challenges
Understanding Balance Control in Parkinson’s
Symptoms vary widely and can affect motor and non-motor functions. Motor symptoms only appear after 60%-80% of cells producing dopamine are lost. Non-motor symptoms, such as cognitive changes or mood disorders, can predate motor symptoms by many years. People with Parkinson’s often experience varying effects to medication, including an on-off phenomenon where a person could alterate between an “on” state, where Parkinson’s impairments are alleviated and an “off” state, characterized by bradykinesia (slow movements) and rigidity

Unique & Individualized Progression
Progression of Parkinson’s Disease
Symptoms vary among individuals, making each case unique. There’s a saying: “If you know one person with Parkinson’s, you know one person with Parkinson’s.” The following is a hypothetical example of the progression of PD over a course of years:
- Swinging of the right arm diminishes.
- Hands begin to curl but can still function as needed.
- The swing of the other arm begins to decrease.
- Shorter steps become necessary.
- Posture changes, including leaning forward or stooping over.
- Tremors develop in the right hand.
- Toes turn into each other while walking.
- Knees and elbows stay bent and don’t fully straighten.
How is Parkinson’s Diagnosed?
Diagnosis of Parkinson's Disease
Diagnosing Parkinson’s relies mainly on clinical assessments. Criteria focus on motor symptoms such as bradykinesia, rigidity, and tremors, along with autonomic dysfunction. These symptoms also have significant overlap with other neurodegenerative processes.

Improving Quality of Life
Treatment Options for Parkinson’s Disease
While there’s no cure, or any known intervention that may slow its progression, treatment aims to manage symptoms and improve quality of life. Medications like corbidopa/levodopa help replace dopamine, but can become less effective over time and can even increase the risk of dyskinesia.
Surgical interventions such as deep brain stimulation, which involves placing an electrode into a specified region of the basal ganglia, can provide relief in selected cases. Although not entirely understood, in well-selected cases there can be dramatic improvements in tremor, bradykinesia, and rigidity, along with reduced medication needs. Exercise therapy plays a crucial role in managing symptoms and preventing fails and is a hallmark of the NeuroPongTM program.